Video
Residency Program
Learn more about the culture of the IU School of Medicine Otolaryngology Residency Program.
Simulation Opportunities
Numerous simulation activities exist for our residents throughout the year including the following:
- Annual one-week long cadaveric national anatomy and surgical course covering all aspects of otolaryngology with invited national speakers and residents from around the country and world in attendance
- Annual skull base simulation courses
- Annual facial trauma plating course
- Temporal bone drilling course occurs throughout the year every week
- Pediatric airway simulation course in the IU Health Advanced Simulation Lab
Focus on Surgical Experience
A high volume of surgical procedures is a notable strength of the Department of Otolaryngology residency program at IU School of Medicine. Upon completion, a resident will have performed approximately 2,500 cases in comprehensive otolaryngology services and specialties within a very diverse patient population. This makes us one of the highest volume surgical experience otolaryngology residencies in the country.
An emphasis on hands-on instruction allows each resident to gain experience in patient care and to begin crafting his or her surgical skills immediately beginning in the first year of residency. Residents are challenged to participate in the process of intraoperative decision-making and are considered active members of the treatment team.
“We recognize that people who are satisfied with their educational experience will approach each day willing and motivated to work hard to advance the field of medicine. We promote an environment of collegiality to respect and encourage our residents within this program.”
Taha Shipchandler, MD, Otolaryngology Residency Program Director
Global Experience
Several opportunities are available at IU School of Medicine for otolaryngology residents to volunteer and train in resource-limited communities outside of the United States. Residents have participated in Vietnam Facial Plastics, Nicaragua Facial Plastics (cleft lip and palate) and the AMPATH consortium in Eldoret, Kenya, for head and neck, facial plastics, otology and general otolaryngology.
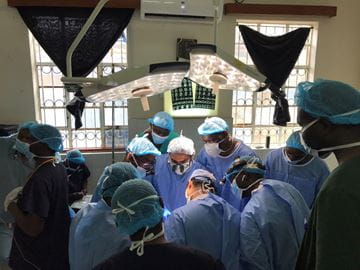
AMPATH—a partnership between Moi University, Moi Teaching and Referral Hospital, North American universities led by Indiana University and the Kenyan Government—is among the largest collaborative health care efforts in the world. At any given time, dozens of IU School of Medicine faculty physicians from various specialties are practicing medicine in Eldoret, Kenya. Otolaryngology faculty and residents participate to treat head and neck tumors, thyroid disease, cleft lip and palate, facial deformities and hearing loss during multiple trips per year. Residents who participate in treating underserved populations receive funding support from the department.
Clinical Facilities
During the program, each resident rotates through otolaryngology—head and neck surgery services at hospitals affiliated with IU School of Medicine in Indianapolis, which include IU Health University and Methodist Hospitals (large quaternary care teaching hospital with Level 1 trauma), Riley Hospital for Children at IU Health, Sidney & Lois Eskenazi Hospital (county hospital), Richard L. Roudebush Veterans Affairs Hospital, IU Health North and West Hospitals (suburban) and various outpatient surgery centers. The variety of health care settings exposes residents to the full breadth and depth of patient diversity, socioeconomic classes, race and ethnicity.

Clinical experience varies at the different sites, but residents have substantial operative involvement and are responsible for monitoring pre- and post-operative care. In some locations, residents may encounter a concentration of tertiary-care problems and procedures with opportunities to follow patients over time and assess outcomes of various interventions.
Each hospital has an active, multidisciplinary tumor board and residents participate in weekly head and neck combined modality tumor conferences and clinics. This provides opportunities to interact one-on-one with oncologists, radiation oncologists, oral surgeons and patients referred to faculty head and neck surgeons.