INDIANAPOLIS — Research from Indiana University School of Medicine shows how formation of the brain’s characteristic wrinkles may influence how brains are wired.
For more than 50 years, researchers have tried to understand why brain folding—development of the characteristic wrinkles of the cerebral cortex—occurs. While every brain is unique, some brain folding patterns can look quite different for individuals with clinical disorders like autism, schizophrenia, epilepsy or bipolar disorder. With advanced technologies like diffusion tensor imaging (DTI), researchers have been able to see that axons—the wires that connect different areas of the brain— are also different in these individuals.
New research published in Nature Communications and led by Kara Garcia, PhD, assistant research professor of radiology and imaging sciences at IU School of Medicine, explores how mechanical forces within the brain might explain the relationship between brain folding and brain connectivity.
“We know a relationship exists between connectivity and clinical disorders. We know a relationship exists between folding and connectivity. But until this point, theories have not been able to fully explain how this fits together,” Garcia said.
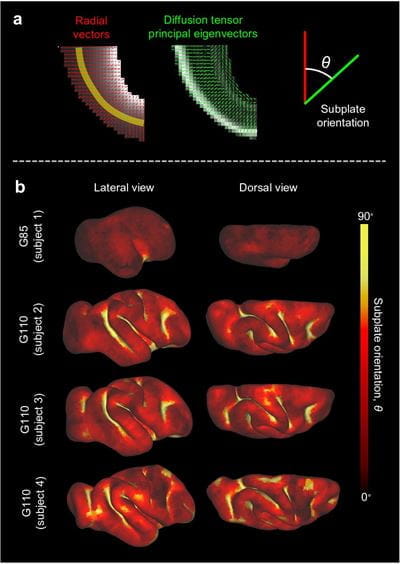
With this new research Garcia and her collaborators, Xiaojie Wang, PhD and Christopher Kroenke, PhD, both researchers at Oregon Health & Science University, have expanded on previous theories for how brain folding and connectivity might be linked. Beginning in utero and up until the first two years of age, the cortex of the brain expands. As this occurs, the brain will bend or buckle, creating folds. Because of this bending effect, the tension between folds can encourage axons—which exist in white matter or the underlying subcortical tissue of the brain— to grow in specific ways, resulting in U-shaped fibers.
While previous theories have suggested the cause for some clinical disorders might be these U-shaped fibers, Garcia suggests that mechanical forces can explain how the brain is organizing into these fiber shapes. Future research could shift its focus to learning why cortical expansion induces folding in the first place, therefore affecting white matter structure.
“If we can understand this cascade of effects, and the biological mechanisms driving all of it, we can better understand the possibilities for targeted early intervention,” Garcia said.
This recent publication also brings to light the ground-breaking research happening at IU School of Medicine regional campuses across Indiana, including Evansville where Garcia is based. Technological advances occurring throughout the state create with them bridges between rural communities and innovative research. This connection not only enables more research in the future but can often be crucial when it comes to health care knowledge, access and prevention for all Hoosiers.
The work was supported by the National Institutes of Health, award numbers R01 NS111948 and R01 AA021981, and the National Science Foundation, award DMS-2011274.
###
About IU School of Medicine
IU School of Medicine is the largest medical school in the U.S. and is annually ranked among the top medical schools in the nation by U.S. News & World Report. The school offers high-quality medical education, access to leading medical research and rich campus life in nine Indiana cities, including rural and urban locations consistently recognized for livability.