Caring for the Caregivers
Matthew Harris Feb 09, 2023
After flying in from Indiana, Daryl insisted on taking their rental car to the store for some ice cream—even though it was getting dark. Once, he’d had an unwavering sense of direction. But, at 61, he’d begun missing turns, even when his wife Mona had just called them out.
He’d been gone quite a while when the phone rang. Trying to navigate the once familiar streets, he’d gotten disoriented. “Can you get me back?” he asked. Using an iPad, Mona navigated him to their condo.
The next morning, Daryl ventured out to the pool to sunbathe. Usually, Mona kept an eye on him from a balcony, but she stepped inside for just a moment. When she returned, he was gone. As she prepared to search for him, Daryl returned. “You’re never going to guess what I did,” he told her. “I got off on the wrong floor, and I was at the wrong room, standing there for 20 minutes.”
Mona burst into tears.
THAT WAS EIGHT years ago. Today, Daryl is among an estimated 6 million Americans and 130,000 Hoosiers diagnosed with Alzheimer’s disease, according to the Alzheimer’s Association. By 2050, as baby boomers age, those numbers are expected to double.
The progression of Daryl’s disease ushered Mona into her own group: family members overseeing the care of a loved one.
Up to 26 million Americans fill that role. Among people over 65, one in three is a caregiver. According to a 2020 AARP study, almost 15 percent of them assisted someone with Alzheimer’s disease.
Indiana University School of Medicine has emerged as an international leader in Alzheimer’s research. Researchers design mouse models that mimic late-stage disease for labs. They refine brain imaging techniques, collect and share samples of brain tissue, search for drug therapies, and study early-onset Alzheimer’s.
Then there are faculty like Nicole Fowler, PhD, and Greg Sachs, MD, who are focused on people like Mona. Their goal: ease the strain on caregivers and ensure families and the health care system provide patients with the best care possible.
“Caregiving is such a prolific aspect of society now,” said Fowler, director of research for the Division of General Internal Medicine and Geriatrics. “It’s hard to imagine not talking about it in the context of goals that we have as a health care system.”
Tending to a family member is never easy but, for those caring for someone afflicted by a neurodegenerative disorder, the strain is high. They not only get a person out of bed, usher them to the restroom, and dress them for the day. They provide transportation, oversee medical care, and manage finances.
Unlike other chronic conditions, the ebb and flow of Alzheimer’s is as distinct as the patient, keeping caregivers on alert and constantly adapting. All while its insidious pathology weathers away the person they love. It’s why 53 percent of caregivers experience severe emotional distress, per the AARP’s data. “They’re not able to interact with you anymore,” Fowler said. “You experience that loss of a person long before their physical body dies.”
As Mona puts it, “You’re a widow before you’re a widow.”
To address such situations, Sachs launched a project using a $3.5 million grant from the National Institute on Aging to help caregivers. Called IN-Peace, it would offer some participants assistance from a nurse and a social worker. Daryl’s neurologist offered it as a potential lifeline.
To Mona, it had the potential to help her build a reliable support system. The Pecks weren’t destitute, but Mona needed help with referrals and finding an in-home aide. If the research helped people in a similar position, all the better. They applied, and she prayed they’d be one of the 50 percent chosen to get help.
Their prayer was answered.
Each month, a nurse and a social worker check in on Mona. They assist with advanced care planning, navigating the health care system, and arranging resources like in-home health aides.
Mona embodies a profile sketched in cold statistics: a woman in her 60s tending to a spouse transitioning to late-stage Alzheimer’s. She gets periodic help from her daughter Kimberly. Yet, percolating beneath it is a clear disparity. “Caregiving, in general, winds up being a woman’s issue,” Fowler said.
In addition to Sachs’ study, Fowler is exploring how a diagnosis affects the mental health of caregivers. Often, it triggers anticipatory grief, an early form of mourning that lingers until a patient’s death. She’s found that, for caregivers, it’s not a passive state: Anticipatory grief raises their stress level, impairs problem-solving, and leads to second-guessing their own decisions, even good ones.
Fowler devised a remote therapy program to combat anxiety and depression, which affects 60 percent of people within two years of caregiving. That small study showed a significant reduction in symptoms—gains that remained six months after a caregiver’s final session.

MONA PECK’S DAYS have a familiar rhythm. Each morning, she rouses Daryl from his sleep in their Anderson home, gets him out of bed and sanitizes the air cushion that prevents bed sores. Since late summer, Daryl, now 69, has become incontinent. Sometimes an aide—who visits two days a week—helps him to the bathroom.
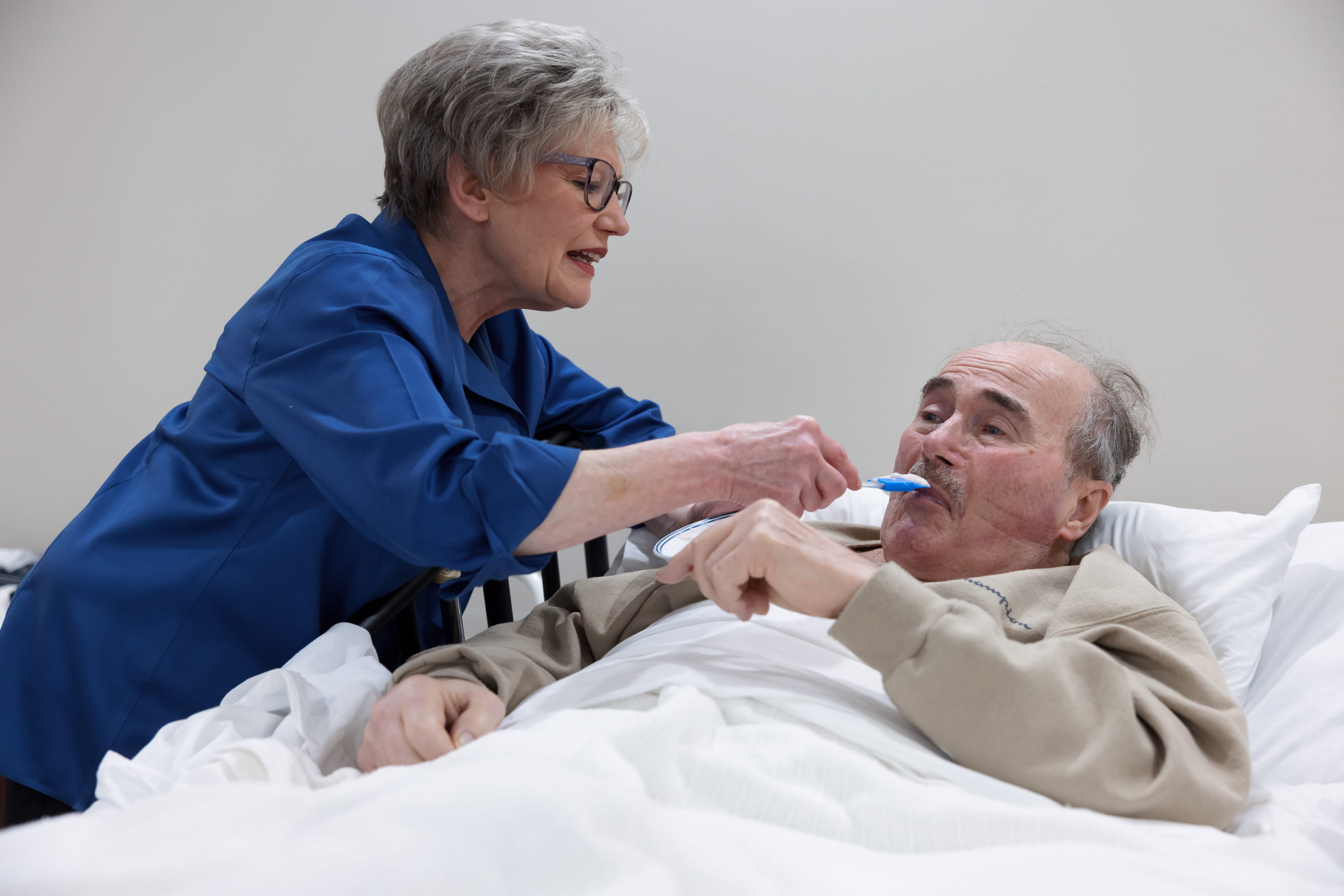
The routine includes a sponge bath, teeth brushing, shaving, and dressing. They usher him to the family room—a task complicated by Daryl’s knee and hip problems. Once seated, they pack in pillows for cushioning. As the aide changes bed linens, Mona serves Daryl a meal from a rolling cart.
Occasionally, she turns on a Cincinnati Reds game. Once, Daryl could pluck arcane baseball statistics from mid-air. Now, he listens silently. “For a while, we did crossword puzzles,” Mona said. “He’s not very interested in them these days.”
Mona still sees the man she married 49 years ago when he was a young maintenance electrician at a General Motors plant outside Cincinnati. He had a quick wit, a love of fun, and a deep faith. When they moved to Anderson, a company town for the auto giant, they raised a daughter. Daryl coached his grandsons in Little League. And they often set off on road trips near and far, including the excursion to Florida.
Once the Pecks returned from Florida, Daryl scheduled a checkup with his primary care physician. An MRI didn’t reveal the tau plaques that are a hallmark of Alzheimer’s. But Daryl’s symptoms and family history—his parents each had dementia—led to a neurological referral. He passed a basic memory test, but his other symptoms led to his grim diagnosis. He asked his doctor if Alzheimer’s would take his life. No, he was told.
“OK,” Daryl said. “I don’t want to end up in the fetal position and die that way.”
Months later, at a couple’s retreat, Daryl had been subdued. He hesitated to share the news. Privately, in their room, he made a request of Mona. “Can we pray the Lord takes me another way?” he asked.
“We simply want him to allow you to pass before it gets to the point I can no longer take care of you,” Mona answered.
EARLY ON, Daryl’s dementia was almost imperceptible. He kept working for three years, and Mona’s workload remained relatively modest. But eventually, the little hacks Daryl used to keep track of tools and projects weren’t enough. When he began misplacing equipment, he retired.
Only then did Mona realize how he’d tried to mask changes. “They hide it,” she said. “And it bothered me that I hadn't been up on it." Soon, Daryl became leery of driving, except to pick his grandsons up from school and making trips to McDonald’s or for Sunday service.
In the meantime, Daryl became unsettled by cognitive changes that warped his reality. On a shopping trip, he stayed in the car while Mona ran inside a store. Upon her return, he pointed to a nearby parked vehicle and said: “Those headrests raised up, turned around, and looked at me. Am I nuts?”
“That’s what your brain perceived,” Mona answered. “That’s going to be happening more.”
Soon, health issues triggered more declines, starting with a hip replacement in 2018. When Mona asked Daryl to raise his left leg, he lifted his right. After a knee replacement, he wouldn’t engage in physical therapy so Mona rehabbed his leg. “It was murderous,” she said.
The family put off two more joint replacement procedures, but painkillers left Daryl in a perpetual fog. After other mobility and balance issues–and falls—he refused to get out of bed. It was too painful. After being hospitalized for COVID in late 2020, he had no peripheral vision. His waning coordination meant he couldn’t eat with either hand. Yet Mona made a pledge.
“I didn’t want his life to change if it did not have to,” she said. Even if it meant trundling a wheelchair everywhere. Or casting a keen eye for seating a short walk from a restroom. They kept up trips to Gatlinburg. They made short excursions to Reds games–even if they left in the middle innings when Daryl got dehydrated. It also unearthed fault lines. When it became too arduous to attend church, Mona queued up a live stream. But Daryl groused: “You never take me anywhere.”

AMY PEMBERTON DOESN'T hesitate when describing Mona’s caregiver traits. “She wants to make sure that what she’s doing genuinely serves Daryl,” she said. “She’s strong in her faith and remains true to who she is.”
Each month, Pemberton, a nurse, and Andrea Vrobel, a social worker, grew to know Mona and her needs well. As part of IN-PEACE's protocol, they oversaw 50 pairs of patients and caregivers.
In real terms, it meant Pemberton placed a phone call to chat about a patient’s behavioral changes, the side effects of medications, and how Alzheimer’s interacts with other chronic conditions. For Mona and others, it meant having a sounding board for dealing with physicians, family members who critique their care, and transitioning a loved one to skilled care. When patients were stable, their check-ins became a chat between old friends. Instead of following strict protocols, they could tailor their approach and act as a coach or consultant.
They are adaptive to the circumstances caregivers confront. They flesh out advanced care plans. They set goals and boundaries for care that match a patient’s values. With that, caregivers feel more confident discussing medical matters, seeking resources, and adapting as a patient’s disease evolves.
For many, it’s a space and time to sit and talk through their concerns and weigh options—with someone who can offer objective insights. “I’m indifferent to the choices you make,” Pemberton said. “I want to give them the risks and benefits.”
Mona’s conversations with Pemberton also rooted her in the reality of Daryl’s disease. “I needed to find out whether I was dealing realistically with everything,” she said.
Pemberton saw that Mona’s devotion might lead her to fixate on little mistakes rather than seeing she was mostly succeeding. “Sometimes,” Pemberton said, “the details can get you fuzzy.”
It’s not uncommon for caregivers. “You’re just kind of stuck in that space,” Fowler said. “You need to have a certain way to reframe your feelings and address them. Throwing more education at those people isn’t going to work. There’s a need to design something that allows them to acknowledge caregiving is hard.”
Fowler implemented a form of teletherapy. Sachs is trying another model that delivers expertise directly to those who need it. It’s distinct in the American health care system, which excels at providing drugs but struggles with behavioral interventions.
Scaling it up is a challenge. Pemberton seeks local partners “close to the ground.” In Indianapolis, it might be CICOA, the state’s largest agency on aging, which funnels home and community-based services to Hoosiers with cognitive disabilities.
Identifying potential partners, however, remains a way off for IN-PEACE. Sachs and his team will need to parse data and publish their findings. And then there’s the question of being able to find and train enough staff. Both Pemberton and Vrobel are unique within their field. Each worked in long-term care facilities and hospital settings. Each has first-hand experience assisting family members diagnosed with dementia, ALS, and Parkinson’s.
Any program based on IN-PEACE could have training modules for coaching and consulting skills. And while that expertise is essential, caregivers place as much importance on the fact that Pemberton has faced the same crisis of confidence and overcome it. “Not just anybody can walk off the street and do this,” she said. “You need professionals that have extensive knowledge, and they need coaching and consulting pieces.”

MONA HARBORS NO illusions about Daryl’s future. There are times when bad days outnumber good ones, when he refuses to eat or acknowledge her presence. Yet there are also fleeting moments when he finds coherence long enough to bestow moments of grace: a kiss on the forehead, a knowing smile. Recently, Daryl reached up and gently stroked the sleeve of her shirt. He leaned forward and whispered.
“I love Mona,” he said.
“Well, Mona loves you, too,” she said.
And a few old habits persist. At night, after slipping a CPAP mask over Daryl’s face, Mona climbs into bed and rests her head on his chest. Then she feels his hand gently stroke her head.
“He knows I’m there,” Mona said. “And I always will be.”
Photo credits: Liz Kaye
Matthew Harris
Matthew Harris is a communications specialist in the Office of Gift Development. Before joining the School of Medicine in 2015, he was a reporter at newspapers in Pennsylvania, Arkansas, and Louisiana. He currently lives in Indianapolis with his wife and two basset hounds.