With advancing battlefield technologies, battlefield medicine, and ever-changing geographical location of military campaigns, military personnel are returning home after facing limb loss. The Indiana Center for Regenerative Medicine and Engineering is committed to helping military personnel lead normal, productive lives and perform activities of daily living that are comparable to people without limb loss. An important secondary goal is to enable the return of affected personnel to full active duty status. At the Indiana Center for Regenerative Medicine and Engineering, scientists and clinicians work with government organizations and industry partners to address pressing military and veteran needs.
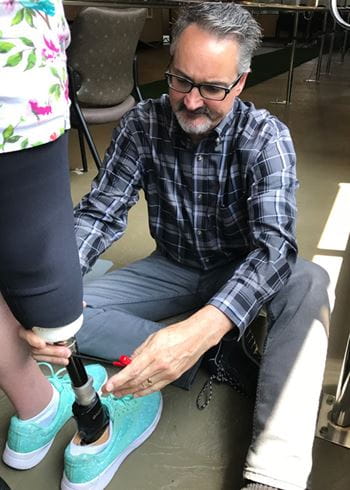
Jeffrey Denune, a clinical research prosthetist, and Sashwati Roy, PhD, professor of surgery with Indiana University School of Medicine, are working to help accomplish the goal of creating a better prosthetic socket to improve residual limb health.
We sat down with Denune to discuss a recent grant from the U.S. Department of Defense that is helping achieve this goal. Jeffrey Denune, a clinical research prosthetist and Sashwati Roy, PhD, professor of surgery with Indiana University School of Medicine, is working to help accomplish the goal of creating a better prosthetic socket to improve residual limb health with the help from a grant from the Deparment of Defense. The grant named Development of Adaptive Vacuum Suspension to Improve Prosthetic Fit and Residual Limb Health” Award to them is the amount of more than $1.9 million.
What is the purpose of the grant that the Indiana Center for Regenerative Medicine and Engineering Medicine received from the Department of Defense?
We are currently in the third phase of the Department of Defense research project. Our primary focus of the project is on residual limb health for amputees, for lower extremity amputees. One of the goals that we're looking at is achieving a comfortable and functional connection between the amputee and their prosthetic socket. That connection is critical to the success of the prostheses, and improving the residual limb health.
What is the issue that people with prosthetics are facing that you are trying to solve?
When an amputee is fitted with a prosthetic device, the residual limb, or the limb that's left after amputation, wasn't designed to be walked on. We were designed to walk on our feet. One of our goals is to fit the most comfortable prosthetic socket design we can for that patient, so they can fully utilize the advanced technology available to them. The fit of the prosthetic socket is critical to the success of the entire prosthetic device.
What are some of the details specific to each patient that are considered when fitting someone for a prosthesis?
Each patient is different and unique, no two are the same. That's what's exciting and challenging about the job. Working with the amputees knowing that every amputee is unique, and every amputee's needs are different. We evaluate each patient differently for those individual’s needs. The technology that we use for patients will vary to that amputee’s needs and environment.
What are some of the issues that amputees face when the prosthesis is not fitting correctly?
There are a couple of issues that can occur when someone is fitted for a prosthetic device. One is that it can be too tight, and that could squeeze the residual limb too much, which can cause discomfort, compromise blood flow or vascularization of the limb. On the other hand, if the prosthesis is too loose, the residual limb can start moving around inside the socket and can cause a wound. Both can be dangerous, especially for patients who have conditions that may compromise their health or their ability to heal wounds properly. Such as those patients who present with diabetes.
 What makes this research unique?
What makes this research unique?
We are doing something different at ICRME. Most funded research goes to support technology—things like microprocessor knees or bionic powered feet. All are important to the user, but I think the area that we're focusing on has been missing. We're focusing on the amputee, and the importance on how they wear that prosthetic device. We want create a smarter connection, so that amputees can simply put on the device, and not have to worry that it will be too tight or get too loose throughout the day. Eliminate the inconvenience of socket adjustments and focus on quality of life.
Why do you think this research is important?
Let's look into and at the world of amputees for a second. Every morning when they get up, they have to put these devices on to get them through the day. We can give them all advanced technology that's very complex, robotic components and sensors. But how effective is that if they can't wear them comfortably? So it's critical that we go the extra mile to help them, put in that extra effort. Help them live a normal life. We need to give them the ability to go through their everyday life. If they need to be able to get up and go to work all day long, then that's what we need to help them do. If their goal is to work all day, come home and play basketball, soccer, or ride bikes with their kids, I think we're obligated to give them that opportunity. That's what this research is doing.