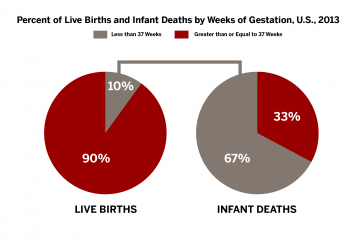
In the United States, Indiana ranks among the highest for the number of babies who die before their first birthday. Despite community involvement and active programs attempting to address factors related to this devastating issue, the state’s infant mortality rate is 20 percent higher than the national average.
Infant mortality is a complex problem. That’s why IU School of Medicine, as part of its strategic plan prioritizing improving population health in Indiana, is partnering with communities throughout the state to address an array of contributing factors—from spacing between pregnancies and maternal care to safe sleep.
Community Health and Social Stability
Twice as many deaths occur in the first year of life than during the next 13 years combined, making infant mortality a leading indicator of a community’s health and social stability. Based on this metric, Indiana is not doing well.
Nationally, the infant mortality rate has decreased over the past ten years—from 6.5 to 5.9 deaths per 1000 live births. While we hope to eventually get to zero, the Healthy People 2020 goal for the United States is 6.0. Indiana, at 7.5—in 2007 as well as in 2016—is still well above that target goal, making this a high-priority issue for the state’s leaders.
In his 2018 State of the State address, Governor Holcomb set a goal to become the best state in the midwest for infant mortality rates by 2024. To help achieve this ambitious goal, IU School of Medicine is working with its clinical partners, including Eskenazi Hospital and IU Health, to address this devastating issue in new ways.