Message from the Program Director

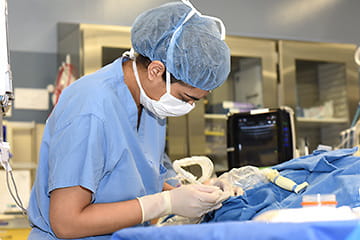
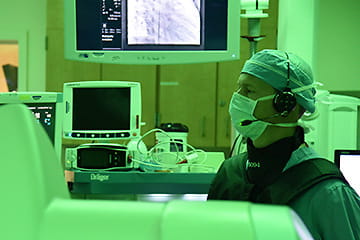
Welcome to the Indiana University School of Medicine Department of Anesthesia Residency program! I am honored to be part of a program that has such a rich history in the advancement of anesthesiology. Having completed my residency training here at IU and now serving as the program director, I can speak firsthand about the exceptional training our residents receive. We have a strong reputation for producing excellent clinicians that go on to contribute to anesthesiology in many ways, including academics, research, and private practice. We take pride in educating our residents by exposing them to a robust number and wide variety of cases that prepares them for any career path they choose. Additionally, our weekly didactics and state of the art simulation center provide supplementary educational tools which help prepare our residents to become board-certified anesthesiologists.
As the program director, I have the honor of advocating for our residents in order to ensure they have a positive experience during their three years with us. Guaranteeing they receive the appropriate clinical and educational experience is only part of the mission, as I also have the privilege to mentor and support this group of young physicians in order to promote resilience and well-being on their path to becoming leaders in the field of anesthesiology. We have an extremely talented and accomplished group of faculty whom I am honored to work with and who are passionate about developing the next generation of anesthesiologists.
Our primary goal is to recruit motivated, bright individuals who share our vision in becoming outstanding clinical anesthesiologists. If you are a medical student seeking an anesthesiology residency that will provide you with an inspiring and supportive environment, I cannot think of a better place to begin your career.
Please don’t hesitate to contact me with any questions.
Jennifer Stewart, DO
Residency Program Director
jlanter@iupui.edu